Salivary gland essentials: What you need to know about salivary cysts, mucoceles, and ranulas
In my many years as a dental professional, I've encountered a lot of cases of mucoceles, ranulas, and salivary cysts. These seemingly innocuous bumps and swellings can sometimes present a diagnostic challenge, and while they are often benign, it's crucial to recognize and understand their underlying causes.
To fully understand these lesions, we must first explore the intricate network of salivary ducts and how they can be vulnerable to various insults and obstructions that can disrupt their integrity, leading to either ductal leakage or obstruction—the root cause of salivary cysts, mucoceles, and ranulas.
Salivary cysts
Salivary cysts (mucous retention cysts type) arise when a salivary gland duct becomes obstructed, typically by a sialolith or a plug of thickened mucus. This obstruction creates a bottleneck, causing mucin to build up within the duct. As the mucin accumulates, the duct expands, forming a cystlike swelling. These cysts tend to occur more frequently in adults and often appear on the upper lip, palate, or buccal mucosa.1,2
Clinically, salivary cysts present as well-defined, fluid-filled swellings that can be moved slightly under gentle pressure. They may occasionally exhibit a subtle yellowish tint due to the trapped mucin. While a salivary cyst might be suspected based on its clinical appearance, a definitive diagnosis requires a biopsy. Histologically, these cysts are distinguished by their characteristic epithelial lining—a layer of cells that encapsulates the mucin within the cyst’s cavity and will rule out other conditions that might mimic a salivary cyst, such as mucoceles, salivary gland tumors, or lymphoepithelial cysts.
Treatment typically involves the surgical removal of the cyst and the affected salivary gland. This approach offers an excellent prognosis, with recurrence being uncommon.
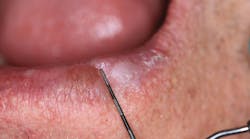
Mucoceles: A common oral lesion
Mucoceles are common oral lesions that develop when the integrity of a salivary duct is compromised. This disruption can arise from trauma, such as lip-biting or accidental injury, or from ductal obstruction due to inflammation, sialoliths, or thick mucus plugs. They primarily affect minor salivary glands, with the lower lip being the most frequent site due to its vulnerability to mechanical trauma during chewing.3 Other contributing factors include chronic inflammation or irritation from heat or smoking and excretory duct fibrosis.
Patients with mucoceles typically present with asymptomatic, painless swellings that develop suddenly, enlarge rapidly, and exhibit fluctuation. Many mucoceles tend to resolve spontaneously as they rupture, and the oral mucosa reabsorbs their contents.
Mucoceles can be further classified based on their underlying mechanism of formation:
- Extravasation mucocele: This is the most common type of mucocele caused by duct trauma that leads to mucin spilling into the surrounding tissues.
- Retention mucocele: This type of mucocele is less frequent and arises from a blockage in the salivary gland duct. Mucin accumulates within the duct, leading to its distension.
In extravasation mucoceles, the leakage of mucin triggers an inflammatory response, resulting in the accumulation of mucin and inflammatory cells, ultimately forming the characteristic fluid-filled swelling.
In retention mucoceles, the obstructed duct experiences mounting pressure due to the impeded flow of saliva. This can eventually cause the duct to rupture, resulting in a mucocele similar to the extravasation type. However, in some cases, the mucin remains confined within the dilated duct, causing a localized swelling.
Clinically, mucoceles typically present as solitary, bluish, translucent, and fluctuant swellings. Histopathological examination reveals a pool of mucin surrounded by granulation tissue and inflammatory cells. Notably, extravasation mucoceles lack an epithelial lining, while retention mucoceles may exhibit a pseudocyst with a lining primarily composed of granulation tissue.4,5
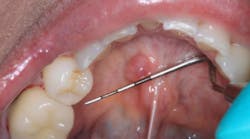
Ranulas: Mucoceles of major salivary gland origin
Ranulas are a specific subtype of mucocele originating from major salivary glands, typically manifesting as fluctuant swellings within the floor of the mouth.6 They are categorized into two types based on their extent and location7:
- Simple (oral) ranula: This pseudocyst remains localized to the floor of the mouth, appearing as a bluish, translucent swelling. It arises from leakage and subsequent accumulation of secretions from a major salivary gland, notably the sublingual gland, above the mylohyoid muscle.
- Plunging ranula: This variant extends beyond the oral cavity, penetrating the mylohyoid muscle to create a deeper swelling in the neck. This occurs as mucus collects and dissects along the fascial planes of the neck.8
Patients with oral ranulas typically present with a painless swelling in the floor of the mouth. This swelling can impact speech, swallowing, mastication, and even respiration as it displaces the tongue upward and medially.9 Sometimes, the tongue’s pressure on the lesion can obstruct salivary outflow, leading to additional symptoms such as pain during eating or chewing.
Managing ranulas can be complex, often requiring a multipronged approach. Treatment options include:
- Marsupialization, which involves creating a surgical opening in the ranula to allow for drainage and to promote healing.
- Excision, which entails the complete surgical removal of the ranula and, in some instances, the associated sublingual gland.
The appropriate treatment modality is selected based on various factors, including the size and location of the ranula, patient preference, and the clinician’s expertise.
Mucoceles, ranulas, and salivary cysts underscore the dynamic interplay between salivary gland function and oral mucosal integrity. It is crucial to differentiate mucoceles from mucous retention cysts, as their management and prognosis may differ. The former lack an epithelial lining and arise from extravasation of mucin, while the latter possess an epithelial lining and result from ductal obstruction.
And now, let’s put all this knowledge to the test.
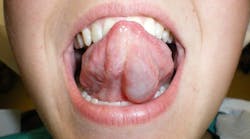
Clinical dental case: Asymptomatic fluid-filled lesions in the vestibular mucosa (nos. 7–10)
Patient presentation: A 17-year-old male patient presented at the initial dental appointment with the following:
Chief complaint: None. The lesions were discovered during a routine oral examination.
Clinical findings:
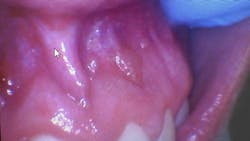
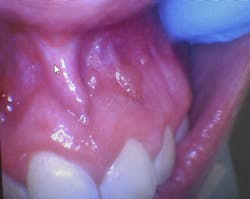
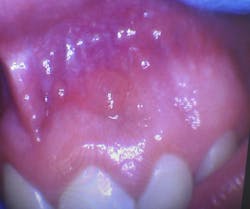
- Seven asymptomatic, fluid-filled lesions
- Lesions ranged in size from 2 mm to 5 mm
- Lesions similar in color to the surrounding mucosa
- Location: vestibular mucosa, in the region of teeth nos. 7–10
Follow-up appointment: Only three of the original lesions remained.
Discussion
The presentation of multiple, asymptomatic, fluid-filled lesions on the vestibular mucosa, with a color similar to the surrounding tissue, further supports the likelihood of a mucocele or a mucous retention cyst. The spontaneous resolution of some lesions further strengthens this hypothesis.
Management
Observation: Given the strong clinical suspicion of mucoceles, the spontaneous resolution of some lesions, and the absence of concerning features, continued observation is appropriate. The patient should be instructed to monitor the remaining lesions and report any changes in size, symptoms, or the development of new lesions.
Biopsy and histopathological examination: If the lesions persist, increase in size, or become symptomatic, a biopsy is indicated to confirm the diagnosis and rule out other possibilities.
Now that you know all this, do you feel confident diagnosing mucoceles or salivary cysts based on the clinical presentation, or would you recommend a biopsy for definitive confirmation?
We welcome your thoughts and perspectives! Let us know what you think about the article’s Instagram post.
Author’s note: This case is intended for educational purposes only and does not constitute medical advice.
Editor’s note: This article first appeared in Clinical Insights newsletter, a publication of the Endeavor Business Media Dental Group. Read more articles and subscribe.
References
- Kundu S, Cheng J, Maruyama S, Suzuki M, Kawashima H, Saku T. Lymphatic involvement in the histopathogenesis of mucous retention cyst. Pathol Res Pract. 2007;203(2):89-97. doi:10.1016/j.prp.2006.11.003
- Kalaimani G, Sivapathasundharam B, Priyadarshini L, Rajeswari M, Karthick BP. Mucous extravasation phenomenon: a clinicopathologic evaluation of 68 cases. J Oral Maxillofac Pathol. 2024;28(2):182-185. doi:10.4103/jomfp.jomfp_373_23
- Bornstein MM, Schriber M, Menter T. [Article in German] Oral retention and extravasation mucoceles of the minor salivary glands – more common than you might think! Swiss Dent J. 2023;133(6):382-383. doi:10.61872/sdj-2023-06-02
- Hayashida AM, Zerbinatti DC, Balducci I, Cabral LA, Almeida JD. Mucus extravasation and retention phenomena: a 24-year study. BMC Oral Health. 2010;10:15. doi:10.1186/1472-6831-10-15
- Elsayed N, Shimo T, Harada F, et al. A challenging diagnosis of a mucocele in the maxillary gingiva: case report and literature review. Int J Surg Case Rep. 2021;84:106030. doi:10.1016/j.ijscr.2021.106030
- Packiri S, Gurunathan D, Selvarasu K. Management of paediatric oral ranula: a systematic review. J Clin Diagn Res. 2017;11(9):ZE06-ZE09. doi:10.7860/JCDR/2017/28498.10622
- Bowers EMR, Schaitkin B. Management of mucoceles, sialoceles, and ranulas. Otolaryngol Clin North Am. 2021;54(3):543-551. doi:10.1016/j.otc.2021.03.002
- Stojanov IJ, Malik UA, Woo SB. Intraoral salivary duct cyst: clinical and histopathologic features of 177 Cases. Head Neck Pathol. 2017;11(4):469-476. doi:10.1007/s12105-017-0810-5
- Choi MG. Case report of the management of the ranula. J Korean Assoc Oral Maxillofac Surg. 2019;45(6):357-363. doi:10.5125/jkaoms.2019.45.6.357
About the Author

Andreina Sucre, MSc, RDH
Andreina Sucre, MSc, RDH, is an international dentist, oral pathology, and oral surgery specialist practicing dental hygiene in Miami, Florida. A passionate advocate for early pathological diagnosis, she empowers colleagues through lectures focused on oral pathologies. Andreina spoke on this topic at the 2024 ADHA Annual Conference, 2023 RDH Under One Roof, and she writes about oral pathology for RDH magazine. Committed to community outreach, she educates non-native English-speaking children on oral health and actively volunteers in dental initiatives.